Shoe Lifts The Podiatrists Option For Leg Length Discrepancy

Leg length inequality goes typically undiscovered on a daily basis, however this issue is very easily solved, and can eliminate quite a few incidents of back ache.
Treatment for leg length inequality commonly consists of Shoe Lifts. These are generally low-priced, generally being under twenty dollars, compared to a custom orthotic of $200 if not more. When the amount of leg length inequality begins to exceed half an inch, a whole sole lift is generally the better choice than a heel lift. This prevents the foot from being unnecessarily stressed in an abnormal position.
Lumbar pain is the most prevalent condition afflicting men and women today. Around 80 million men and women suffer from back pain at some point in their life. It's a problem that costs companies vast amounts of money yearly as a result of time lost and productivity. Fresh and superior treatment methods are constantly sought after in the hope of lowering economical impact this issue causes.

Men and women from all corners of the earth suffer the pain of foot ache due to leg length discrepancy. In these cases Shoe Lifts can be of beneficial. The lifts are capable of decreasing any discomfort and pain in the feet. Shoe Lifts are recommended by numerous skilled orthopaedic orthopedists.
So as to support the human body in a well-balanced manner, the feet have got a significant part to play. In spite of that, it is often the most neglected zone of the human body. Some people have flat-feet meaning there may be unequal force exerted on the feet. This will cause other parts of the body such as knees, ankles and backs to be impacted too. Shoe Lifts make sure that the right posture and balance are restored.
Hammer Toe Treatment In Your Own Home
A Hammer toe is a deformity of the second, third or fourth toes in which the main toe joint is bent upward like a claw. Initially, hammertoes are flexible and can be corrected with simple measures. Left untreated, they can become fixed and require surgery. Hammertoe results from shoes that don?t fit properly or a muscle imbalance, usually in combination with one or more other factors. Muscles work in pairs to straighten and bend the toes. If the toe is bent and held in one position long enough, the muscles tighten and can?t stretch out.
Causes
Hammer toe is often caused by wearing shoes that do not fit properly. If shoes are too small either in length or width, then the Hammer toes toes are held in a shortened position for long periods and the muscles eventually shorten and pull the toes into the bent position. Alternatively it can be caused by overactivity in the extensor digitorum dongus muscle (right) and a weakness in the counteracting muscle under the foot, such as flexor digitorum longus. Sometimes it can be a congenital condition, meaning it is present from birth. It is also more common in those with arthritis in the foot or diabetes.
 Symptoms
Symptoms
Pain on the bottom of your foot, especially under the ball of your foot, is one of the most common symptoms associated with hammertoes. Other common signs and symptoms of hammertoes include pain at the top of your bent toe from footwear pressure. Corns on the top of your bent toe. Redness and swelling in your affected area. Decreased joint range of motion in your affected toe joints.
Diagnosis
Most health care professionals can diagnose hammertoe simply by examining your toes and feet. X-rays of the feet are not needed to diagnose hammertoe, but they may be useful to look for signs of some types of arthritis (such as rheumatoid arthritis) or other disorders that can cause hammertoe. If the deformed toe is very painful, your doctor may recommend that you have a fluid sample withdrawn from the joint with a needle so the fluid can be checked for signs of infection or gout (arthritis from crystal deposits).
Non Surgical Treatment
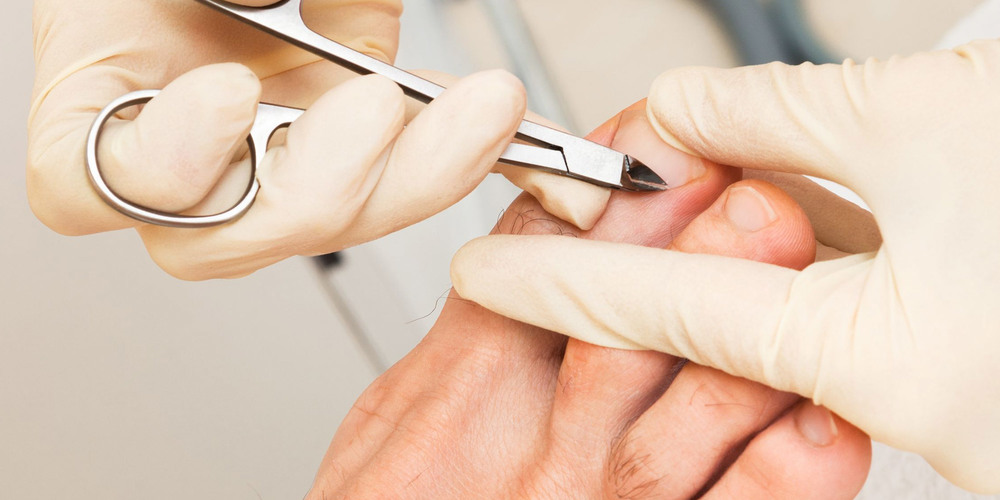
If the toes are still mobile enough that they are able to stretch out and lay flat, the doctor will likely suggest a change of footwear. In addition, she may choose to treat the pain that may result from the condition. The doctor may prescribe pads to ease the pain of any corns and calluses, and medications ranging from ibuprofen to steroid injections for the inflammation and pain. Other options for non-surgical treatments include orthotic devices to help with the tendon and muscle imbalance or splinting to help realign the toe. Splinting devices come in a variety of shapes and sizes but the purpose of each is the same: to stretch the muscles and tendon and flatten the joint to remove the pain and pressure that comes from corns.
Surgical Treatment
Joint resection procedures involves removing part of one of the two small joints of the toe directly underneath where the digit is crooked. The purpose is to make room for the toe to be re-positioned flat or straight. Because hammer toes become rigid or fixed with time, removing the joint becomes the only option when the knuckle is stiff. Its important to understand that this procedure does not involve the joint of the ball of the foot, rather the a small joint of the toe. Medical terminology for this procedure is called a proximal interphalangeal joint arthroplasty or a distal interphalangeal joint arthroplasty, with the latter involving the joint closer to the tip of the toe.
What Are The Primary Causes Of Bunions?
Overview
 Bunions, Corns, and Calluses are common foot ailments associated with improperly-fitted footwear. Please contact your family doctor or Podiatrist to ask them how Birkenstock footwear or arch supports can help treat your symptoms. Also, feel free to contact your local Birkenstock retailer about their healthy footwear recommendations. Birkenstock has many products that can help with Bunions, Corns, and Calluses. Bunions are a prominent bump on the inside of the foot around the big toe joint. Corns are an accumulation of dead skin cells usually found on the toes, forming thick hardened areas. They contain a cone-shaped core whose point can press on a nerve below causing pain. Calluses are also an accumulation of dead skin cells that harden and thicken over an area of the foot. They are the body?s defense mechanism against excessive pressure and friction. Calluses are normally found on the bottom of the foot, the heel, and/or the inside of the big toe.
Bunions, Corns, and Calluses are common foot ailments associated with improperly-fitted footwear. Please contact your family doctor or Podiatrist to ask them how Birkenstock footwear or arch supports can help treat your symptoms. Also, feel free to contact your local Birkenstock retailer about their healthy footwear recommendations. Birkenstock has many products that can help with Bunions, Corns, and Calluses. Bunions are a prominent bump on the inside of the foot around the big toe joint. Corns are an accumulation of dead skin cells usually found on the toes, forming thick hardened areas. They contain a cone-shaped core whose point can press on a nerve below causing pain. Calluses are also an accumulation of dead skin cells that harden and thicken over an area of the foot. They are the body?s defense mechanism against excessive pressure and friction. Calluses are normally found on the bottom of the foot, the heel, and/or the inside of the big toe.
Causes
Bunions are among the most common problems of the foot. They are several possible reasons a bunion may develop, though a biomechanical abnormality (improper function of the foot) is the most common cause. In an unstable flat foot, for example, a muscular imbalance often develops that, over time, causes bunions. Bunions tend to run in families, and most podiatrists believe that genetic factors play a role in predisposing some people to develop bunions. Poor shoes, like high heels and pointed toe boxes--exacerbate the condition by speeding up the development of bunions, and by making bunions more painful. Poor shoe choices is at least one of the reasons bunions are much more common in women than men.
Symptoms
Many people do not experience symptoms in the early stages of bunion formation. Symptoms are often most noticeable when the bunion gets worse and with certain types of footwear. These include shoes that crowd the toes and/or high-heeled shoes. When symptoms do occur, they may include physical discomfort or pain. A burning feeling. Redness and swelling. Possible numbness. Difficulty walking.
Diagnosis
The doctor considers a bunion as a possible diagnosis when noting the symptoms described above. The anatomy of the foot, including joint and foot function, is assessed during the examination. Radiographs (X-ray films) of the foot can be helpful to determine the integrity of the joints of the foot and to screen for underlying conditions, such as arthritis or gout. X-ray films are an excellent method of calculating the alignment of the toes when taken in a standing position.
Non Surgical Treatment
Most bunions can be treated without surgery. The first step for treating bunions is to ensure that your shoes fit correctly. Often good footwear is all that is needed to alleviate the problem. Shoes that are wide enough to avoid pressure on the bunion are the obvious first step. Look for shoes with wide insteps and broad toes and definitely no high heels. Sometimes, you can get your existing shoes stretched out by a shoe repairer. Seek advice from a podiatrist. Pads and toe inserts. Protective bunion pads may help to cushion the joint and reduce pain. Toe inserts are available that splint the toes straight. It may be recommended that you wear some orthotics to improve your foot position when walking. Medicines. Some people find anti-inflammatory medicines, such as ibuprofen or aspirin, or paracetamol help ease the pain of their bunions. 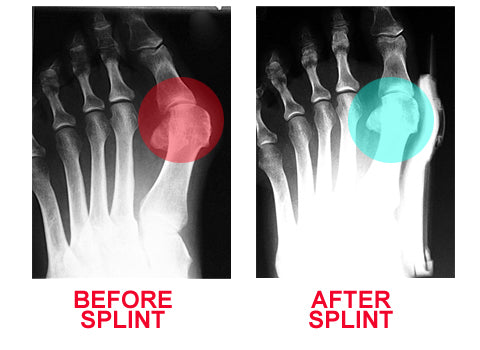
Surgical Treatment
Arthrodesis involves fusing together two bones in your big toe joint (metatarsophalangeal joint). The procedure is usually only recommended for people with severe deformities of the big toe joint, which make it too difficult for doctors to completely fix the joint, or when there's advanced degeneration of the joint. After arthrodesis, the movement of your big toe will be severely limited and you won't be able to wear high heels. An excision arthroplasty involves removing the bunion and the toe joint. A false joint is created by scar tissue that forms as a result of the operation. The procedure involves pinning the joint in place with wires, which will be removed around three weeks after surgery is carried out. An excision arthroplasty can only be used in certain circumstances, and is usually reserved for severe, troublesome bunions in elderly people.
Prevention
Here are some tips to help you prevent bunions. Wear shoes that fit well. Use custom orthotic devices. Avoid shoes with small toe boxes and high heels. Exercise daily to keep the muscles of your feet and legs strong and healthy. Follow your doctor?s treatment and recovery instructions thoroughly. Unfortunately, if you suffer from bunions due to genetics, there may be nothing you can do to prevent them from occurring. Talk with your doctor about additional prevention steps you can take, especially if you are prone to them.
Achilles Tendon Injury Treatment Exercises
Overview
 Achilles Tendon Rupture Surgery is a surgical procedure is used to repair a ruptured Achilles tendon. There are two types of surgery an open surgery and a percutaneous surgery, in both cases the surgeon sews the tendon back together through the incision helping the tendon to heal properly and restore function to the foot and ankle. If the injury or rupture has caused severe swelling the surgery may be delayed for a short period of time to allow the swelling to go down.
Achilles Tendon Rupture Surgery is a surgical procedure is used to repair a ruptured Achilles tendon. There are two types of surgery an open surgery and a percutaneous surgery, in both cases the surgeon sews the tendon back together through the incision helping the tendon to heal properly and restore function to the foot and ankle. If the injury or rupture has caused severe swelling the surgery may be delayed for a short period of time to allow the swelling to go down.
Causes
Your Achilles tendon helps you point your foot downward, rise on your toes and push off your foot as you walk. You rely on it virtually every time you move your foot. Rupture usually occurs in the section of the tendon located within 2 1/2 inches (about 6 centimeters) of the point where it attaches to the heel bone. This section may be predisposed to rupture because it gets less blood flow, which also may impair its ability to heal. Ruptures often are caused by a sudden increase in the amount of stress on your Achilles tendon. Common examples include increasing the intensity of sports participation, especially in sports that involve jumping, falling from a height, stepping into a hole.
Symptoms
It is important to know that pain at the back of the heel is not always due to Achilles tendon rupture. It may be due to bursitis (fluid accumulation in the heel due to repeated irritation) and tendonitis (pain along the Achilles tendon due to constant friction and irritation). The above disorders tend to improve with use of pain medications and rest, whereas Achilles tendon rupture requires surgery and/or a cast.
Diagnosis
The diagnosis is usually made on the basis of symptoms, the history of the injury and a doctor's examination. The doctor may look at your walking and observe whether you can stand on tiptoe. She/he may test the tendon using a method called Thompson's test (also known as the calf squeeze test). In this test, you will be asked to lie face down on the examination bench and to bend your knee. The doctor will gently squeeze the calf muscles at the back of your leg, and observe how the ankle moves. If the Achilles tendon is OK, the calf squeeze will make the foot point briefly away from the leg (a movement called plantar flexion). This is quite an accurate test for Achilles tendon rupture. If the diagnosis is uncertain, an ultrasound or MRI scan may help. An Achilles tendon rupture is sometimes difficult to diagnose and can be missed on first assessment. It is important for both doctors and patients to be aware of this and to look carefully for an Achilles tendon rupture if it is suspected.
Non Surgical Treatment
Non-surgical treatment of Achilles tendon rupture is usually reserved for patients who are relatively sedentary or may be at higher risk for complications with surgical intervention (due to other associated medical problems). This involves a period of immobilization, followed by range of motion and strengthening exercises; unfortunately, it is associated with a higher risk of re-rupture of the tendon, and possibly a less optimal functional outcome. 
Surgical Treatment
Unlike other diseases of the Achilles tendon such as tendonitis or bursitis, Achilles tendon rupture is usually treated with surgical repair. The surgery consists of making a small incision in the back part of the leg, and using sutures to re-attach the two ends of the ruptured tendon. Depending on the condition of the ends of the ruptured tendon and the amount of separation, the surgeon may use other tendons to reinforce the repair. After the surgery, the leg will be immobilized for 6-8 weeks in a walking boot, cast, brace, or splint. Following this time period, patients work with a physical therapist to gradually regain their range of motion and strength. Return to full activity can take quite a long time, usually between 6 months and 1 year.
Prevention
Achilles tendon rupture can be prevented by avoiding chronic injury to the Achilles tendon (i.e. tendonitis), as well as being careful to warm up and stretch properly before physical activity. Additionally, be sure to use properly fitting equipment (e.g. running shoes) and correct training techniques to avoid this problem!